|
Although not all patients were screened for thrombosis, this complication was diagnosed in symptomatic patients with the use of ultrasonography. However, in this study, thrombosis occurred in only one patient (1.0%), which is a lower rate than those in previous studies, suggesting that PICC is sufficiently safe to replace CVC. In fact, the rate of symptomatic thrombosis with PICC is reportedly 1–25% and is considered to be the most common complication of PICC. According to these results, the CLABSI rate was lower even with a longer duration of catheter use in the PICC group, suggesting that PICC can be used safely in the ICU.Īlthough PICC is reported to be safe due to the lower infection rate, it is not superior to CVC because of the higher rate of complications, such as thrombosis. Additionally, the median duration of catheter use was significantly longer in the PICC group than in the CVC group (16 vs. However when the analysis was limited to patients for whom the catheter was changed for the first time in the ICU after CVC insertion in the ER with similar indication and catheter insertion times, the CLABSI rate was significantly lower in the PICC group than in the CVC group (10.3 vs. Although the CLABSI rate was lower in the PICC group than in the CVC group, this difference was not statistically significant. Our results were somewhat higher than those in previous studies. 
In the present study, there was a difference in the CLABSI rate between the PICC and CVC groups (9.1 vs. The discrepancies in the CLABSI rate and duration of catheter use among institutions is thought to be related to the catheter care bundle, the compliance to guidelines by medical staff, and the department where catheterization was performed. 1.3–5.2/1,000 catheter-days, respectively) and the difference in the duration of catheter use between the PICC and CVC groups (19–23 vs. However, it remains unclear whether PICC is beneficial for hospitalized patients, as several studies have reported that PICC is not superior to CVC due to the similarity in CLABSI rates (1.3–2.3 vs. reported a lower CLABSI rate with PICC than with CVC in the surgical ICU (2.2 vs. reported a lower CLABSI rate with PICC than with CVC (4.2% vs. In addition, PICC is considered to be associated with a lower CLABSI rate than CVC. PICC is a special type of CVC that was first introduced by Hoshal and has since been used increasingly in the hospital setting due to the ease of insertion into the peripheral vein, greater patient satisfaction, and improved safety. 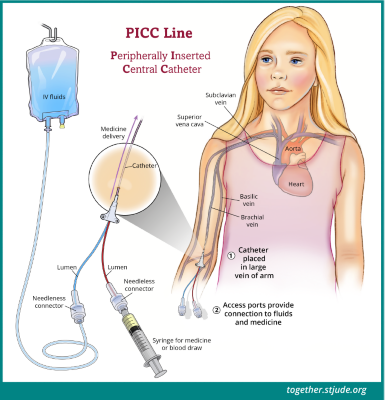
CVC is a reliable intravenous route for the delivery of inotropic drugs, hypertonic fluids, blood products, and total parenteral nutrition to acutely ill patients, as well as for hemodynamic monitoring and blood sampling. The CLABSI rate and duration of catheter use among trauma patients were compared between the CVC and PICC groups to determine whether PICC meets the goals of a lower infection rate and long-term use. Therefore, the present study aimed to compare the rate of bloodstream infections and duration of catheter use between conventional CVC and PICC to determine whether PICC meets the goals of a lower infection rate and long-term use for trauma patients. Also, PICC may be a more appropriate method for outpatients than inpatients, although there is no general consensus. 
On the other hand, the incidence of complications is higher with PICC than with CVC, although no significant difference in bloodstream infection rates has been reported. In addition, PICC can be used for longer periods with lower risks of bloodstream infection than conventional CVC, so its use in the hospital setting has continued to increase over the past two decades. 
A peripherally inserted central catheter (PICC) is a special type of CVC with insertion into a vein in the arm rather than in the neck or chest to avoid mechanical complications that may occur during conventional CVC. However, CVC is associated with an increased risk of bloodstream infection, which may prolong the length of hospital stay and adversely affect patient morbidity and mortality. Central venous catheter (CVC) plays a fundamental role in the acute setting of trauma patients, as it is a reliable intravenous route for the delivery of various therapeutic fluids, as well as for hemodynamic monitoring.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
